What is Follicle Stimulating Hormone
Follicle Stimulating Hormone (FSH) is one of the gonadotrophic hormones, and the other is a Luteinizing Hormone (LH). The pituitary gland releases both into the bloodstream and the body. Follicle Stimulating Hormone (FSH) is one of the hormones essential for the development function of women’s ovaries and men’s testes. In women, Follicle Stimulating Hormone (FSH) stimulates the growth in the ovary before the release of an egg from one follicle to the ovulation. It also increases estradiol production. In men, Stimulating Follicle Hormone (FSH) acts on the Sertoli cells of the testes to stimulate sperm production (spermatogenesis).
How is Follicle Stimulating Hormone (FSH) controlled?
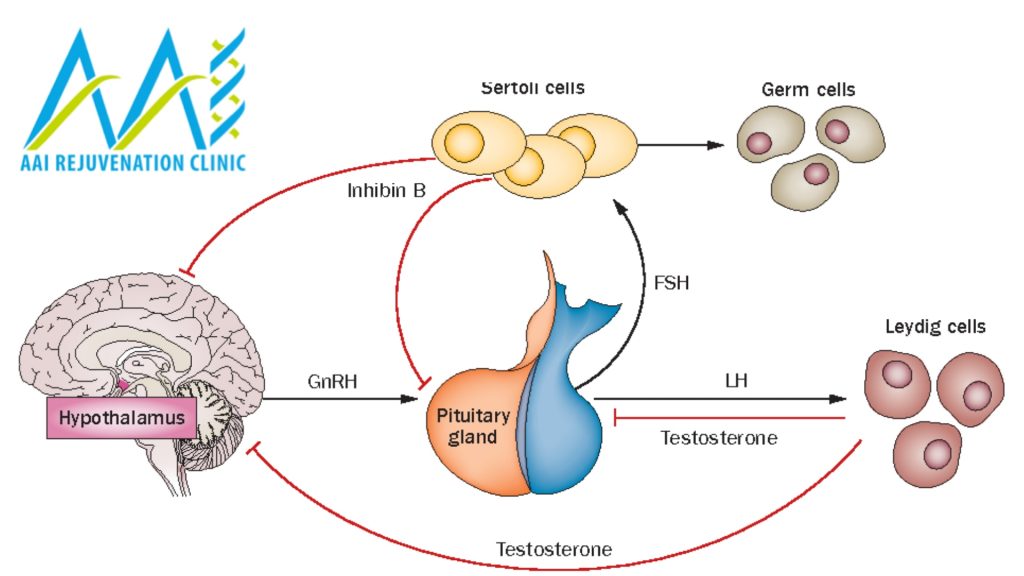
The release of Follicle Stimulating Hormone (FSH) is regulated by the levels of some circulating hormones released by the ovaries and testes. This system is called the hypothalamic–pituitary–gonadal axis. The gonadotropin-releasing hormone is published in the hypothalamus and the receptors in the anterior pituitary gland to stimulate both the synthesis release of Follicle Stimulating Hormone (FSH) and Luteinizing Hormone (LH).
The released Follicle Stimulating Hormone (FSH) is carried in the bloodstream and binds to receptors in the testes and the ovaries. Using this mechanism Follicle Stimulating Hormone (FSH), along with Luteinizing Hormone (LH), can control the functions of the ovaries and testes. In women, when hormone levels are deficient, and it complicates the menstrual cycle, this is sensed by nerve cells in the hypothalamus.
These cells produce the more gonadotrophin-releasing hormone, which stimulates the pituitary gland to produce more Follicle Stimulating Hormone (FSH) and Luteinizing Hormone (LH) and release these into the bloodstream. The rise in Follicle Stimulating Hormone (FSH) stimulates the follicle’s growth in the ovary, and the cells of the follicles produce increasing amounts of estradiol. In turn, this production of these hormones is sensed by the hypothalamus and pituitary gland, and less gonadotrophin-releasing hormone and Follicle Stimulating Hormone (FSH) will be released. However, as the follicle grows, and more and more estrogen is produced from the strands, it simulates a surge in luteinizing hormone (LH) and Follicle Stimulating Hormone (FSH), which stimulates the released egg from a mature follicle – ovary.
During women’s menstrual cycle, there is a rise in the Follicle Stimulating Hormone (FSH) secretion in the first half of the period, which stimulates follicular growth in the ovary; after ovulation, each month, the ruptured follicle forms and Corpus luteum that produces high levels of progesterone. This inhibits the release of stimulating Follicle Stimulating Hormone (FSH), and towards the end of the cycle, the Corpus luteum breaks down, and progesterone production decreases. The next menstrual period begins when Follicle Stimulating Hormone (FSH) starts production again and returns to normal…
Now In men, the production of Follicle Stimulating Hormone (FSH) is regulated by levels of testosterone and inhibin, both produced by the testes. Follicle Stimulating Hormone (FSH) regulates testosterone levels. When this rises, they are sensed by nerve cells in the hypothalamus so that gonadotropin-releasing hormone secretion and, consequently, Follicle Stimulating Hormone (FSH) is decreased. The opposite occurs when testosterone levels drop. This is known as a ‘Negative Feedback in the body’ control, so testosterone production remains steady. But the sensed by cells in the anterior pituitary gland rather than the hypothalamus.
What happens if you have too much Follicle Stimulating Hormone (FSH)?
Often raised levels of Follicle Stimulating Hormone (FSH) are a sign of malfunction in the ovary or testis. If the gonads fail to create enough estrogen and testosterone and inhibit the proper feedback control of Follicle Stimulating Hormone (FSH), production from the pituitary gland is lost. The levels of both Follicle Stimulating Hormones (FSH) will rise. This condition is called hypogonadotropic-hypogonadism and is associated with primary ovarian failure or testicular failure.
This is seen in states such as Klinefelter’s syndrome in men and Turner syndrome in women. In women, Follicle Stimulating Hormone (FSH) levels also start to rise naturally around the menopausal period, reflecting a reduction in the function of the ovaries and a decline in estrogen and progesterone production. There are rare pituitary conditions that can raise the levels of Follicle Stimulating Hormone (FSH) in the bloodstream.
This overwhelms the regular negative feedback and can cause ovarian hyperstimulation syndrome in women’s ovaries. Symptoms include enlarging the ovaries and potentially dangerous fluid accumulation in the abdomen, triggering a rise in ovarian steroid output. This leads to pain and other problems in the body’s pelvic area.
What happens if you don’t produce enough Follicle Stimulating Hormone (FSH)?
In women, lack of Follicle-Stimulating-Hormone (FSH) leads to incomplete development in puberty o poor ovarian function (ovarian failure). In this situation, ovarian follicles do not grow properly and do not release in the egg, thus leading to infertility. Since levels of Follicle-Stimulating-Hormone (FSH) in the bloodstream are low, this condition is called hypogonadotropic-hypogonadism. This condition is called Kallman’s syndrome, associated with a reduced sense of smell. Sufficient Follicle-Stimulating-Hormone (FSH), this action is also needed for proper sperm production in men in case of complete absence of Follicle Stimulating, and the lack of puberty and infertility due to no production of sperm is called (azoospermia).
Partial Follicle-Stimulating-Hormone (FSH) deficiency in young men can also cause delayed puberty and low sperm production (oligozoospermia), but fathering a child may still be possible. Follicle-Stimulating-Hormone (FSH) occurs after puberty; there will be a similar loss of fertility…
**NOTE** The content in this blog is subject to interpretation and is the opinion of the content writer. We do not claim it to be fact. We encourage you to consult a medical doctor before taking any prescribed medications or supplements.
Conclusion
Supporting Hormones health is essential for overall well-being and vitality. By incorporating regular exercise, proper nutrition, adequate sleep, stress management techniques, and IV therapy, you can help maintain optimal testosterone levels and lead a healthy, balanced life. Always consult a healthcare professional before making significant changes to your lifestyle or starting any new treatments to ensure they suit your needs.
At AAI Rejuvenation Clinic, we advise anyone to think seriously about beginning Hormone treatment if there is no medical need for it. However, we will take every precaution to ensure that you read your program’s positive benefits by providing the latest at-home hormonal mouth-swab testing to ensure we are continually monitoring your progress and aware of any adverse side effects. Fill out the Medical History Form, or if you need more information, call us at (866) 224-5698 or (866) AAI-Low-T.
Low Hormone Symptoms
- Motivation
- Sex Drive and Desire
- Depression
- Fatigue
- Erectile Dysfunction
- Cholesterol
- Low Energy
- Memory Loss
- Osteoporosis
- Wounds & Illness
- Muscle Mass
- Sleep Disturbances
- Thyroid Dysfunction
- Weight Gain